Universal Health Coverage is a conversation driven by discourse on removing financial barriers in access to health care for the most marginalised populations: who is covered, what services are covered and how financing for these groups and these services will be accomplished.
Sexual and reproductive health, on the other hand, has always been a conversation driven by discourse on ‘access’ which includes tackling the non-financial barriers: availability, acceptability, affordability, quality of services; discrimination; and inequalities caused by structural and social barriers such as gender, class, ethnicity, caste, sexual orientation and migrant status.
Hence we as advocates and activists cannot automatically assume that both these discourses will converge, and previous advocacy on the inclusion of a comprehensive SRH pack will be integrated at country level.
In recent meetings, it has become apparent that the models touted – talk about the concept of ‘pooled’ funds – some services free and fully funded or co-funded by governments, some services funded by a variety of payment schemes. In traditional insurance or payment schemes – only risks can be assessed and included – and pregnancy is almost always termed as ‘non-random’ and high probability for women unless the payment schemes are large enough to ensure effective risk pooling and cross subsidising.[1]
However, in many developing countries like my own which has seen a burgeoning of insurance schemes – Malaysia aims to have high health insurance coverage – something like 75-80%; but still contraception, abortion and maternal delivery services not covered by most private insurance schemes! So we have to be mindful and closely monitor, and look at what SRH services are being included, and what pool of funding is proposed for that particular service. We need to be very clear to governments and donors that UHC coming into play, does not necessarily mean coverage for all types of SRH services,[2] and for all groups of people.
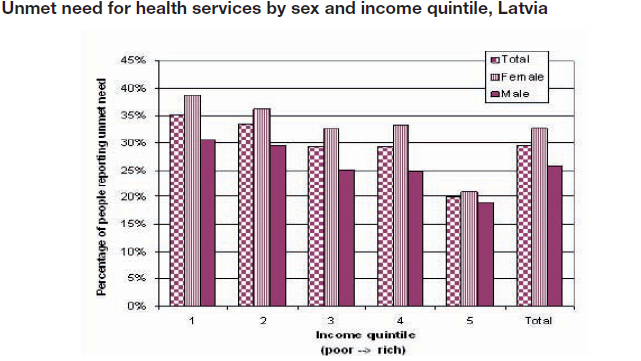
In a recent seminar to ARROW staff, Dr Sundari Ravindran shared how gender is a critical component in health: “It is not only poor women who may have financial barriers to accessing health care; across all wealth quintiles, women have greater unmet need for health services.”[1]
Moreover, UHC at country level is taking place within a context where we see uneven progress towards achievement of SRH across all countries because political will for the comprehensive agenda has been lacking. At country level, SRH is a field dominated by battles over gender equality (autonomy and bodily rights in particular) and socio-economic inequity (who gets what services).
SRH subjects touch the most intimate part of life, relationships touched by this – and none so divided between ‘ideal’ behaviour and ‘real’ behaviour. In the past – this ideal perpetrates gender norms and presumption – sex is for pro-creation, rather than pleasure; sex is occurring within marriage, and that sex is heteronormative. In this, will UHC reinforce the perpetration of these ‘ideals’ in sexual and reproductive health behavior or will it address the socio-economic and gender imbalances in order to reach those who are really marginalised?
What we already know is that marginalised women populations from rural, poor, lesser educated backgrounds, caste and indigenous status, face barriers of discrimination, receive fewer options, are not able to receive quality services – and even when they receive services could die as shown in Chattisgarh,[3] Koppal[4] – or face provider violence and coercion.
For particular groups, there are formal laws or informal rules which restrict access and discriminate against them which further marginalises them and deepens their oppression. For example, across a number of countries, female migrant workers face immediate deportation when found pregnant; migrants with HIV status not able to obtain work permits. Laws and rules like these drive migrant workers to hide their health status and not seek timely medical attention. Low skilled migrant workers are usually not covered by health insurance packages, and may have little or no access to even basic contraception unless they pay for it from their own pockets.
Unless there is concerted effort UHC may also replicate and tighten existing social norms and social sanctions around sexuality. In the Asian region, state defined sexuality is usually heteronormative, and occurring within marriage. Some states are moving towards criminalising premarital and extra-marital sexuality such as Brunei recently did. Within such frameworks even unmarried young people will not be able to receive adequate SRH services. Some states also offer conversion therapy programmes for LGBT persons. Unless there is effort to correct some of these adverse paradigms prevalent at national level SRH service provision, UHC implementation may turn up meaning very little for the marginalised people we care most about.
We must think about designing and developing a health system that is inclusive, that recognizes the needs of those marginalised, that takes account of laws and policies, while changing norms on the grounds, because UHC itself will not address challenges around rights, access, participation and inclusion. Where is the space to do that?
by Sivananthi Thanenthiran
[1] Ravindran, Sundari. “Universal Health Coverage: Making health systems work for all?”
[2] SRH services cover an ambit of services as defined by the ICPD including information, counseling, services for contraception, safe delivery, abortion, infertility, RTIs, STIs including HIV/AIDs, cancers such as breast, cervical, uterine, endometrial, active discouragement of FGM/C.
[3] https://indianexpress.com/article/india/chhattisgarh-sterilisation-tragedy-two-and-a-half-years-deaths-of-13-mothers-later-4605460/
[4] http://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.605.2179&rep=rep1&type=pdf


